
Shared Risk.
Shared Rewards.
Better Experience.
Working together to take control and gain leverage.
Take control. Pool risk. Gain Scale.
Captivated Health® brings together forward‑thinking employers who believe in a better way to deliver dependable, cost‑effective health benefits. By pooling risk and creating collective scale, members gain the power of collaboration while maintaining full control over their plans. Through shared risk management, stop‑loss protection for high‑cost claims, transparent data insights, and member‑led governance, the platform ensures accountability, stability, and sustainable savings over time.

The game is not broken. It’s just not designed for you to win. The “new” game for mid-market organizations is called a Captive.
How the Captivated Health Platform works
Health insurance is an employers second largest expense — yet many employers settle for the “less bad” annual renewal. Captivated Health helps mid‑market organizations take control, reduce volatility, and gain purchasing leverage through pooled risk, smarter design, and transparent vendor accountability.
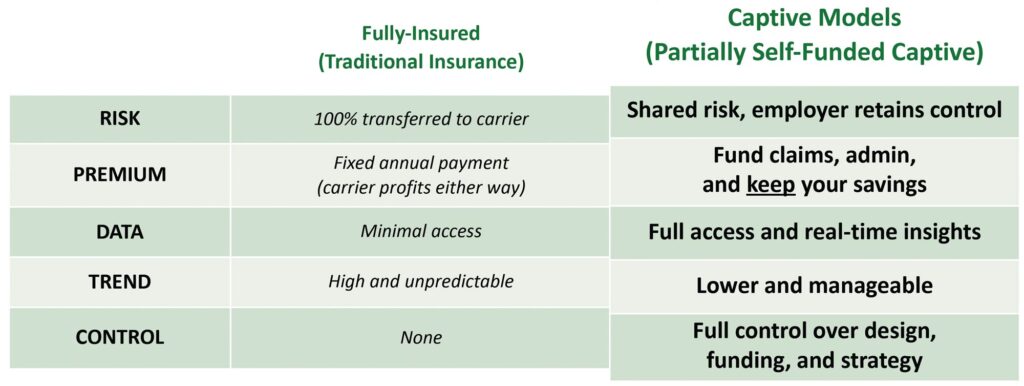
Traditional Model vs. Captive Model
Traditional Insurance
Captive Solution
Captivated Health helps members take control by moving from system-decision to self decision.
Health Insurance Financing The Captive Way
Health insurance is typically the organization’s second‑largest, fastest‑rising expense. By pooling similar employers, a captive creates scale, lowers fixed costs, and improves predictability for major claim events. The Captivated Health Platform acts as a high‑cost claim “shock absorber,” so no single plan sponsor bears the full financial exposure of high-cost claims.
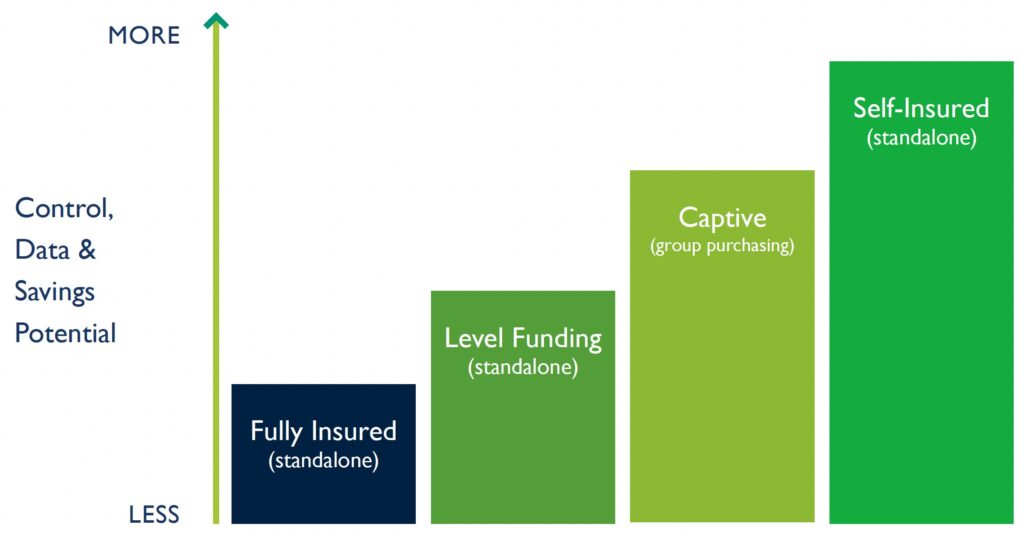
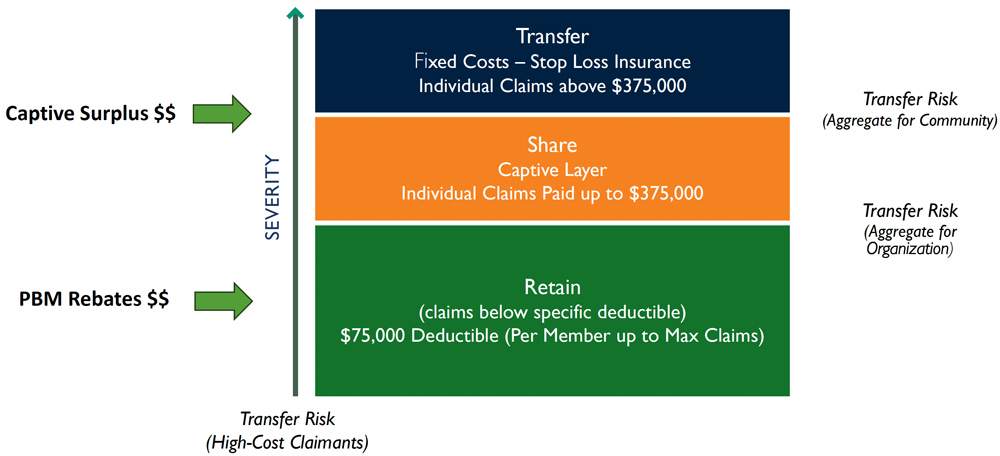
How The Captive Model Works
People: The #1 Asset To Any Organization.
Rising health insurance costs drain resources from your business and your people. The Captivated Health platform removes inefficiency from benefits so you can reinvest savings where they matter most—employee wellbeing, retention, and growth. Our platform turns health insurance plan expenses into a strategic asset on your balance sheet, not just a line item.
Changing The Rules
A Clearer Path from Cost Center to Strategic Asset

What we expect:




